Carl Cincinnato
This expert interview is from a recent interview at the Migraine World Summit. For more information visit: www.migraineworldsummit.com
Menstrual migraine attacks tend to be more severe, disabling, and more refractory compared to other attacks. They also affect about half of all women with migraine. Can these attacks be managed? What strategies are available for people like us with menstrual migraine? And what factors help you determine the best approach?
These questions and more are answered by Dr. Anne MacGregor, a professor at Barts and The London School of Medicine & Dentistry, U.K. Dr. MacGregor is a specialist in headache and women’s health, she’s also a leading researcher in the field of migraine in women and one of the world’s most respected migraine specialists, with over 25 years of clinical experience and 10 books to her credit.
Are hormonal migraine attacks different?
Dr. MacGregor: “Hormonal migraine attacks are different from the attacks that occur at other times of the cycle. Women who are experiencing migraine regularly around the time of their periods will often not realize that they’re migraine attacks because they will just think, ‘Oh, it’s that time of the month again. I’ve got my period. I’ve got these terrible cramps,’ or it’s what’s to be expected to have a headache with it. And they often don’t realize that those attacks that they’ve got are migraine. It’s often then only when they realize that they’re getting similar, but not quite so bad, attacks at other times of the month that they might link the two together. But we often find that women with the hormonal migraine just don’t recognize them for what they are.”
Are hormone level measurements helpful in treating menstrual migraine?
Dr. MacGregor: “Well, we can measure the hormones, but measuring the hormones isn’t going to give us any useful information. Because there’s nothing wrong with the hormones. There’s nothing wrong with the levels, there’s nothing wrong with the drop. It’s exactly the same as every single other migraine trigger. So for example, if you get migraine triggered by going too long without eating or you get migraine triggered by dehydration, there’s nothing wrong with you that those triggers result in a migraine. The difference is that you as an individual are susceptible to those normal changes. So I often get asked, ‘Can’t you measure my hormones? Don’t I need a supplement here? Can’t you add a little bit more on here?’ Doesn’t make the slightest bit of difference. We’re dealing with normal, healthy people and a brain that is just not happy with some of the changes that it’s dealing with, and decides it wants to take a break from them during the migraine attack. So that’s what we’re trying to manage — healthy women’s hormones.”
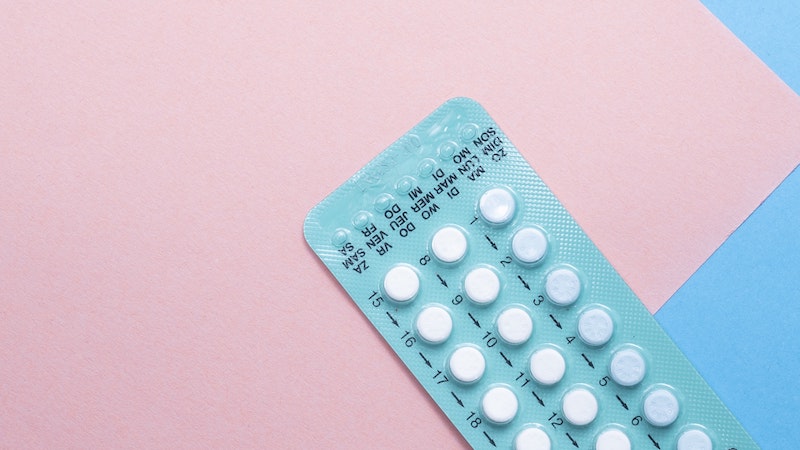
What would be the optimal contraception method for a woman with migraine?
Dr. MacGregor: “There is no optimal contraceptive method for every woman with migraine. It would depend on their needs and benefits. The safest contraceptive, and simplest one, is probably the progestogen-only pill, the desogestrel progestogen-only pill that inhibits ovulation but it doesn’t completely shut down all ovarian activity. So it can be very beneficial at helping all menstrual migraine or menstrual attacks of migraine in a majority of women, but not all women, who take it; the main side effect being unscheduled bleeding, which can itself be linked with migraine, again. Many women are very happy with a combined pill, which contains estrogen and progestogen, but the estrogen has a slightly negative side, and women who are at high risk of developing blood clots from making their blood a little bit more sticky can’t take it. But in healthy users, they can take it up until the age of 50. So it’s not the drugs that are dangerous; it’s not the hormones we give that are dangerous. It’s finding out whether the woman is safe to take those particular hormones, and exactly the same with migraine treatment. Not every migraine treatment can be taken by everybody. It’s the person who has the dangers, not necessarily the drug. You have to match the two.”
Watch the full interview to find out:
How many women have hormonal migraine?
What is the relationship between hormonal migraine and other types of migraine?
Is it possible to effectively manage menstrual migraine?
Is there a standard treatment for menstrual migraine or should it be customized to each individual?
Which hormones are involved in hormonal migraine and how does their involvement impact treatment?
How can NSAIDs be used in symptomatic treatment and prevention of menstrual migraine?
What role can contraceptives play in treatment of hormonal migraine?
Why is record-keeping so important to treatment when a woman suspects hormonal migraine?
What is the connection between migraine and other conditions such as endometriosis, polycystic ovary syndrome, or hypothyroidism?
What are the safety considerations related to stopping periods as a treatment for menstrual migraine?
What factors affect transgender patients in use of hormonal therapy in migraine treatment?
Watch Dr. Anne Macgregor’s interview preview here or order it as part of the Migraine World Summit package from this page.
If you previously purchased the 2019 Migraine World Summit, you are all set to login to watch the full interview.